Traditional rules of thumb in healthcare planning have changed. Once-accepted rules can now be the wrong course to take for healthcare institutions looking to maintain and grow their competitive position in the marketplace.
Whether in urban or rural setting, development costs for new facilities a major concern. Facility operating costs also have gone through the roof, in part because healthcare environments have become more complex and need uninterruptible power sources and upgraded information system technology. Stricter government regulations and standards of care that are more reliant on sophisticated data and medical equipment have also forced the non personnel costs of medical institution operations to rise.
In light of these societal, economic and social changes, health facility planners and administrators need to revisit their strategic thinking about future facility changes and expansions.
So, what are the new thumb rules an institution should follow when undergoing a facility master planning exercise? A few salient ones to consider are presented here.
PARADIGM SHIFT IN APPROACH
In today’s Healthcare scenario each Specialty desires its own entrance, image, and identity. Like the retail industry, which has moved from aisles of merchandise to numerous mini-boutiques within departments, hospitals are moving away from the image of a monolithic medical provider where all healthcare is under one roof. Hospitals are touting their specialties, boutique practices, and celebrity physicians, and the terms differentiation, repositioning, and branding have entered the healthcare provider’s dictionary
As a result, facility planning rules have changed. Let us look at some of the parameters that can be identified as Thumb Rules for developing an Efficient, Patient friendly Healthcare Facility.
DESIGN PARAMETERS FOR PATIENT CENTERED CARE
The essential theme for Patient – Centered Care is that healthcare should be delivered in a manner that works best for patients.
- PATIENT’S VALUES AND NEEDS
-
- Providing adequate privacy to patients during examination and discussion by providing proper screens / separate rooms for examination and treatment as well as counseling rooms near OT and ICU for discussion
- Movement of in-patients from rooms/wards to treatment/diagnostic areas through separate corridors, other than used by visitors minimizes patient discomfort
- Providing of ramps with proper 1:10 / 1:8 slopes – even stairs are to design with uniform steps all thru the facility to prevent fall during movement of people
- Providing of accessible toilets for Patients – senior citizens and the differently-able d
- Designing a “way-finding” process into every project both Indoor and Outdoor. Patients, visitors, and staff all need to know where they are, what their destination is, and how to get there and return. Making spaces easy to find, identify, and use without asking for help
- PATIENT’S COMFORT
-
- Provide spacious room to reduce crowding
- Providing proportionate size and scale of room with use of non-reflective finishes in cheerful and varied colours
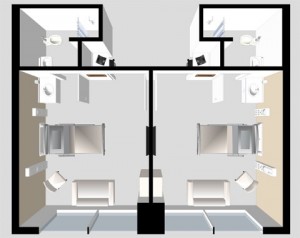
- Provide each patient a variety of spatial experiences, including access to a garden or a day space – 2 slides (for this point)
- Providing views of the outdoors from every patient bed, or photo murals of nature scenes are helpful where outdoor views are not available
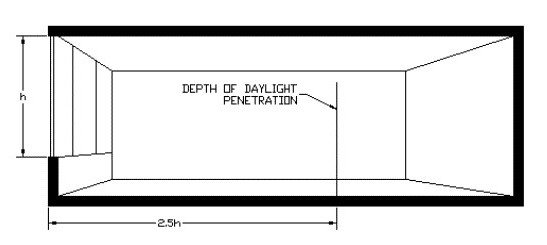
- Providing Natural light — The distinction between daylight and electrically lit spaces is significant — Daylight intensity levels are in the range of 10,000 to 40,000 lux, while a brightly lit interior averages between 300 and 500 lux.
Benefits:
-
- Daylight can reduce a patient’s post surgical recovery time. The human biological clock or the circadian system plays an important role in maintaining the well-being
- Studies show that “ICU psychosis”, a state of delirium experienced in critical care environments, is dramatically reduced when spaces are day lit
- Research shows that physical and visual connections to the natural environment assists in patient recovery and healing, reduce stress, and improve the overall health care environment
- Staff is also benefitted thus leading to improved delivery of services to the patients they serve
 DESIGN PARAMETERS FOR OPTIMISATION
DESIGN PARAMETERS FOR OPTIMISATION
The designs of new healthcare facilities need to be flexible enough to cope with changing patient expectations, new treatments and medical advances. Healthcare facilities space is used by a wide range of user groups including clinical and support staff, patients and their relatives, volunteers and visitors. This has created the need for multi-use and multi-functional healthcare facility space, which forms a key parameter to optimize the design of healthcare spaces. The need is for multi-use and multi-functional space, flexible planning and standardization.
- DESIGN FLEXIBLE SPACES
- Modular concepts of space planning
- Design of generic bay sizes for patient rooms / OT / ICU so as to be able to accommodate these spaces optimally within the planning grid
- Where size and program allow, design on a modular structural and engineering systems. For large projects, this provides continuing adaptability to changing programs and needs if properly planned and designed.
- Open-ended corridor spaces, with well planned directions for future expansion provided flexibility to expand as per need at that time.
- STANDARDIZATION
- Currently standardization has become an important strategy in healthcare facility designs
- It is observed that standardized clinical areas promote efficiency in care and treatment, make life easier for clinical staff and reduce the incidence of medical error
- There are significant relationships between space optimization from a functional perspective and from a construction perspective
Planning for Identical OT’s increases work efficiency for the OT staff during operations as they can retrieve and locate instruments effortlessly
Planning for Identical ICU units improves the response time of ICU staff in emergency situations as the equipments / monitors etc would be located at exactly the same location in each cubicle and hence there is no time loss for locating them
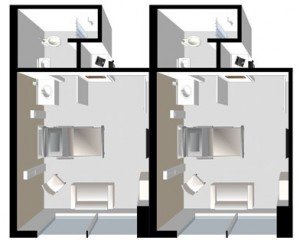
Planning for Identical Nursing rooms also improves staff efficiency to a great extent – however rooms with mirror layouts help optimise for services.
ECO-FRIENDLY DESIGN
- REDUCTION IN NOISE LEVELS
Noise is a well-documented source of stress in health care settings. Noise increases stress levels for patients and caregivers. The WHO recommends that continuous background noise in hospital rooms should not exceed 35 decibels (dB), and night time peaks in patient care areas should not exceed 40 dB. Today, Fenestration is available to keep out the outdoor noise levels. Use of sound insulated partitions and false ceilings help reduce indoor noise levels and prevent transfer of sound from one space to the other.
- IMPROVING INDOOR AIR QUALITY
The importance of good air quality in controlling and preventing airborne infections in healthcare facilities cannot be overemphasised. Providing clean, filtered air and effectively controlling indoor air pollution through ventilation are two key aspects of maintaining good air quality.
-
- High-efficiency particulate air (HEPA) filters, in particular, are highly effective in filtering out harmful pathogens and are strongly recommended in areas housing immune-compromised patients.
- Adequate ventilation rates as per NABH standards and regular cleaning and maintenance of the ventilation system are critical for controlling the level of pathogens in the air. The Operation theatres and ICU set-ups in particular need to have minimum 2-stage filtration system. The patient rooms may / may not have air conditioning but necessarily need to have ventilation prescribing to the requisite air changes.
- Some special precautions to prevent infection during periods of construction and renovation like installing barriers between patient care and construction areas is recommended
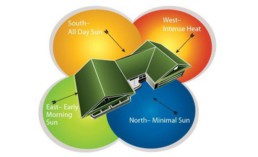
- BUILDING ORIENTATION
Well-orientated buildings maximise daylighting through building facades reducing the need for artificial lighting. In the equatorial location, if solar heat gain is to be avoided, the main windows should face north. Solar heat gain on the west side can be particularly troublesome as its maximum intensity coincides with the hottest part of the day. In urban buildings with an east or west orientation, where there is a demand for large openings, a special glazing that reduces solar heat gains should be chosen. Provision of proper sun-shading devices to every external opening of the building according their orientation is essential.
SUSTAINABLE DESIGN
It is important to Design Sustainable Hospitals to improve on operational efficiency and reduce working costs. As we saw earlier the building itself needs to be planned to maximise on functionality also while choosing on the aesthetic features such as glazing careful choices need to be made.
- BUILDING FABRIC
Building Fabric protects the building occupants and plays a major role in regulating the indoor environment. It is a major factor in determining the amount of energy a building will use in its operation. Solar heat gains can be controlled by the sensible sizing and positioning of the glazed surfaces taking the orientation into consideration. Selecting glass appropriately – like heat – reflective glass helps in conserving energy.
- CONSERVE WATER AND ELECTRICITY
- Take advantages of gravity flow where possible for distribution of water supply
- Use rain water harvesting or Ground water recharge system – which is mandatory to be provided for hospitals
- Installation of a sewage treatment plant
- Reuse storm water or gray water for non potable applications
- HIGH EFFICIENCY FITTINGS — Use of LED light fittings and Energy Efficient Equipment – for Medical and AC
- SOLAR POWER — Include solar panels or photovoltaic cells on the roof and generate electricity and heat water for hospital use from the sun’s energy alternately the panels could be used to generate power for back –up lighting or street lighting
These are a few thumb rules that I believe would add value to our projects – from a Patient as well as a Doctor’s perspective – also taking into account the GREEN aspect there-by making the facilities COST-EFFECTIVE at an operational level and also help reduce the CARBON footprint for the project.
Reference:
- New Planning Rules of Thumb for New Hospitals : April 1, 2006 by Gary Vance, AIA, ACHA and Scott Radcliff.
- HaCIRIC – excerpts from research synopsis of — Developing an integrated approach to the design of high quality healthcare space using Modelling, Simulation and Visualisation (MSV)
- Hospital Health care facilities – Whole building design guide.htm, article by Robert F Carr.
- AE DESIGN II – BUILDING OPTIMIZATION – rule of thumb for window configuration.
By Ar. Kshititi Nagarkar
SHREE DESIGNS
Related Posts
Designing Healthcare Facilities
Negative Pressure Rooms in Hospitals
Negative pressure rooms (NPRs) may occupy a small footprint in a hospital, but their performance…
Designing Healthcare Facilities
Designing for Night-Shift Healthcare Workers
Hospitals run 24/7, but most design decisions are made with daytime workflows in mind. We’ve been…
Designing Healthcare Facilities
The Science of Hospital Windows
Windows in hospitals do far more than bring in light; they influence recovery rates, infection…
Infographic,Designing Healthcare Facilities
How Design Impacts Patient Care
Ever wondered what goes into designing a hospital or clinic that truly works - for doctors, staff,…
Designing Healthcare Facilities
Textures in Healthcare Spaces
When designing hospitals or clinics, texture is often seen as a “finishing touch.” At Shree…
Designing Healthcare Facilities,Infographic
The Lifecycle of a Healthcare Facility Design
Ever wondered what goes into designing a hospital or clinic that actually works - clinically,…
Designing Healthcare Facilities
Designing NABH-Compliant Hospital Interiors
A well-designed hospital isn’t just about aesthetics. From fire safety and infection control to…
Designing Healthcare Facilities,Infographic
Blueprint for Healthcare Design
From room dimensions to lighting levels, every detail matters in healthcare design. At Shree…
Designing Healthcare Facilities
Building Better Day Surgery Centres
Efficient care, happier patients, and smarter workflows - this is what defines a successful…
Designing Healthcare Facilities,Infographic,Project Management
Designing Healthcare Spaces That Truly Heal
From concept to completion, every medical space we design prioritizes patient flow, staff…
Designing Healthcare Facilities
The Business of Wellness
In the $1.8 trillion wellness industry, first impressions matter. Patients don’t just choose a…
Designing Healthcare Facilities
Efficient Hospital and Clinic Design
India’s emerging cities are growing rapidly, creating an urgent demand for accessible and efficient…
Designing Healthcare Facilities
Creating Calming and Confidential Spaces for Fertility Clinics
As the demand for fertility treatments grows, the architecture of these clinics plays a vital role…
Designing Healthcare Facilities
Designing the Perfect Hospital Pharmacy
Hospital pharmacies are the backbone of seamless patient care. From efficient workflows to secure…
Designing Healthcare Facilities
Preventive Care Facility Design Strategies
With preventive care emerging as the future of healthcare, this post outlines key architectural…
Designing Healthcare Facilities
Thermal Comfort Decoded
Thermal comfort plays a critical role in patient recovery, staff productivity, and overall…
Designing Healthcare Facilities
Building for Tomorrow: The Imperative of Adaptable Healthcare Design
Healthcare facilities need to be as dynamic as the industry itself. Traditional, rigid designs can…
Designing Healthcare Facilities
Designing Single Speciality Healthcare Centres
As single-speciality centres grow, their design needs become more specific, calling for tailored…
Designing Healthcare Facilities
Innovative Design Solutions for Senior Care Facilities
Designing senior-friendly spaces in healthcare facilities is crucial for catering to the evolving…
Designing Healthcare Facilities
Designing a Dental Clinic for Success
Providing quality dental care is not just about the technical elements of the treatment. It's also…
Designing Healthcare Facilities
3 Essential Design Features for Intensive Care Units
ICUs are not just limited to single units housing all critical patients. If the facility has…
Designing Healthcare Facilities
3 Lessons Learned While Building a Cardiac Cath Lab
Cardiac care design is moving at the sound of a new beat! The number of Cath labs in India has…
Designing Healthcare Facilities
5 Essential Elements of Healthcare Design
Design makes a significant impact on the delivery of care for both healthcare providers and…
Designing Healthcare Facilities
5 Best Ways to Create Healing Spaces for Kids
Designing spaces in healthcare facilities tailor-made for children is a lesson in balance! A…
Designing Healthcare Facilities
Top 5 Trends in Healthcare Design
Design can make all the difference when it comes to improving patient care. From a patient’s point…
Designing Healthcare Facilities
The Architectural Design of Hospital Facilities
Shree Designs designed and executed many efficient and safe healthcare setups in the middle of the…
Designing Healthcare Facilities
Dauntless Designers
Healthcare Radius in its 7th Anniversary Special issue in October 2019, featured a "power list of…
Designing Healthcare Facilities
The changing face of healthcare design
After completing a decade in designing healthcare projects, Kshititi Nagarkar, principal architect,…